What’s Your NPS?
This article was originally published in the Open Minds Daily Executive Briefing on 06/01/22.
www.openminds.com
By Monica E. Oss, Chief Executive Officer of OPEN MINDS
Like all executives, I’m always looking for benchmarks of ‘how we are doing’ compared to other organizations. The most common organizational performance measure have been financial—margin, cash flow, and earnings before interest, taxes, depreciation, and amortization. But since the advent of the four-quadrant ‘balanced scorecard’ approach in 1992, executives have been pushed to look at more than financial measure.
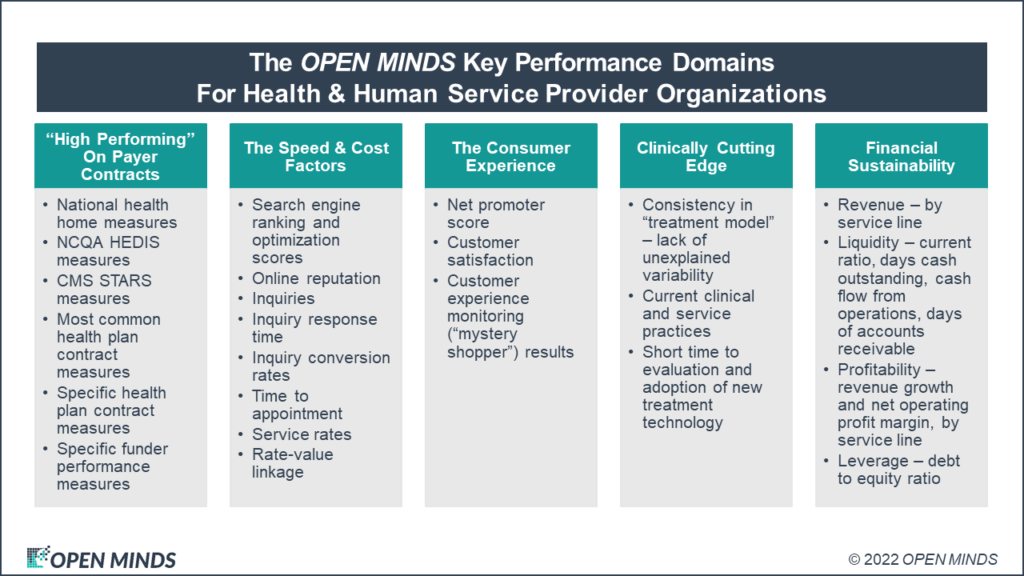
Over the past decade, our team has taken that balanced scorecard concept and evolved it to five key domains for performance measurement and management among health and human service organizations. The domains include:
1. Performance on payer contracts
2. The speed and cost of service
3. The consumer experience
4. Measures of clinical expertise
5. Financial sustainability measures
And in the domain, the consumer experience, net promoter score (NPS) is an important metric—though underutilized in health and human services. If you don’t know what NPS is—or you’ve heard about it but don’t use it—it’s a method used in many fields to determine customer satisfaction and loyalty. NPS is a one-question metric that measure how your organization and its services are perceived by your patients. NPS scores typically range from -100 to +100 (the first being all detractor customers and latter all promoter customers). Many say that any score above zero is technically a good score, while anything above 50 is an excellent score.
Even though NPS is not common in health and human services, it’s very popular with Fortune 1000 companies—currently in use in two-thirds of them. The reason is simple—growth. According to recent estimates, roughly 20% to 60% of organic growth variation can be attributed to NPS, with users outgrowing competitors “by a factor greater than two times.”
The question for executive teams in health and human services considering measuring NPS—or already measuring NPS—is what does NPS data add to executive decisionmaking? I recently spoke with a couple OPEN MINDS Elite members to get a gauge on where they are at with this tool.
 For Maureen Walsh, Chief Advancement & Strategy Officer at St. David’s Center for Child & Family Development, using NPS for reputation management brings three important functions to the table—it’s the clearest measure of consumer satisfaction, it’s a top generator for new referrals, and it’s understandable and valued by payers. St. David’s asks consumers the NPS question across the range of services that a child and/or family receives with a variety of tech tools—including tablets, laptops, POS, text messaging, and e-surveys. The data is analyzed by service.
For Maureen Walsh, Chief Advancement & Strategy Officer at St. David’s Center for Child & Family Development, using NPS for reputation management brings three important functions to the table—it’s the clearest measure of consumer satisfaction, it’s a top generator for new referrals, and it’s understandable and valued by payers. St. David’s asks consumers the NPS question across the range of services that a child and/or family receives with a variety of tech tools—including tablets, laptops, POS, text messaging, and e-surveys. The data is analyzed by service.
“We give multiple ways for parents/guardians to respond just to meet our families where they are and do our best to get a decent response rate,” she explained. “We know we’re speaking a language our payers will understand by capturing it and leveraging it in contracting. Are we leveraging it enough? Not yet. Most of our use of NPS so far from an external value standpoint has been in reporting related to county contracts for case management and day treatment (CTSS services) and philanthropy. Our goal and intention to collect it more consistently and regularly and build a plan to use it optimally is in our strategic plan and a priority for Year One.”
 Becky Olson-Hernandez, Chief Quality Officer for Compass Health also uses NPS and shared the “two prime indicators” that are most important—making sure that consumers get what they need, and making sure Compass Health gets what it needs in terms of referrals.
Becky Olson-Hernandez, Chief Quality Officer for Compass Health also uses NPS and shared the “two prime indicators” that are most important—making sure that consumers get what they need, and making sure Compass Health gets what it needs in terms of referrals.
“First, do our clients believe that they are getting the help that they need and are treated with dignity and respect,” she explained. “Related to this is whether our clients would/do recommend us to their family and friends. The second indicator is whether we receive referrals from our community partners, and whether they acknowledge our expertise and reach out to us as a resource.”
 For Benchmark Human Services, Doug Beebe, President and Chief Executive Officer, notes that reputation management means collecting data from four groups—direct consumers of services and their support systems; existing customers such as health plans and human services agencies; potential customers, including related entities such as schools and law enforcement; and employees and contracted consultants.
For Benchmark Human Services, Doug Beebe, President and Chief Executive Officer, notes that reputation management means collecting data from four groups—direct consumers of services and their support systems; existing customers such as health plans and human services agencies; potential customers, including related entities such as schools and law enforcement; and employees and contracted consultants.
“Each of the four core groups has specific identified or implied data points that are, or can be measured to some degree,” he explained. “Our organization is continuing to develop metrics around these groups. Related to this measurement are variables including differentiation from competitors, ongoing reinforcement of core values and culture, and building a generalized brand awareness. These factors are more difficult to quantify. For example, Benchmark’s persistent focus on embracing supporting persons with complex needs. This has become integral to our reputation and potential growth and is a key differentiator in the human services market. We are developing metrics based on unsolicited inquires, referrals, and identified responses to conference/event-based presentations and exhibits.”
The goal is to document evidence of high quality, innovative services, which Mr. Beebe says is not a strict measurement of reputation but still critical to the process of reputation management. “The willingness to innovate, to understand consumer and employee motivations, respond quickly with operational solutions, collaborate with disparate stakeholders, and focus on practical and/or easily understood strategies with clear return on investment are now essential,” he explained. “We consider these to be key drivers of a compelling reputation.”
The results could be eye-opening—and provide some of the first solid data on customer experience. For executive teams, it is a benchmark on which services are meeting customer satisfaction and which are falling short.

